Your Employee Just Had Surgery. How Do You Know If It Worked?
.png)
Here’s a question most benefits leaders have never been asked: after an employee has surgery, how do you know whether it actually helped?
Not whether it was completed. Not whether they were readmitted. Whether the surgery did what it was supposed to do—reduce their pain, restore their mobility, let them get back to their life.
If you’re relying on the standard signals—claims data, readmission rates, complication flags—you’re seeing the story months after it’s over, and you’re only seeing part of it. There’s a better way. It’s called patient-reported outcome measures, or PROMs, and it’s the quality signal that most of the employer benefits world hasn’t discovered yet.
What PROMs Actually Are
PROMs are standardized questionnaires that ask patients directly about their health status—things like pain levels, physical function, quality of life, and ability to perform daily activities. They’re not satisfaction surveys. They’re clinical tools, developed and validated by researchers, that capture the dimensions of recovery that matter most to the person who had the procedure.
The concept isn’t new. PROMs have been used in clinical research for decades, and since 2009, England’s National Health Service has required them for certain elective surgeries. In the U.S., the Centers for Medicare and Medicaid Services (CMS) already requires PROM collection for some orthopedic procedures, and the FDA recognizes PROMs as acceptable endpoints to support treatment-benefit claims in medical product labeling. CMS has begun incorporating PROM-based performance measures into hospital quality reporting, and stakeholders have discussed expanding their use in other value-based programs.
What’s newer is the idea that PROMs can be collected in real time—during recovery, not months later—and used to actively manage care rather than just grade it after the fact.
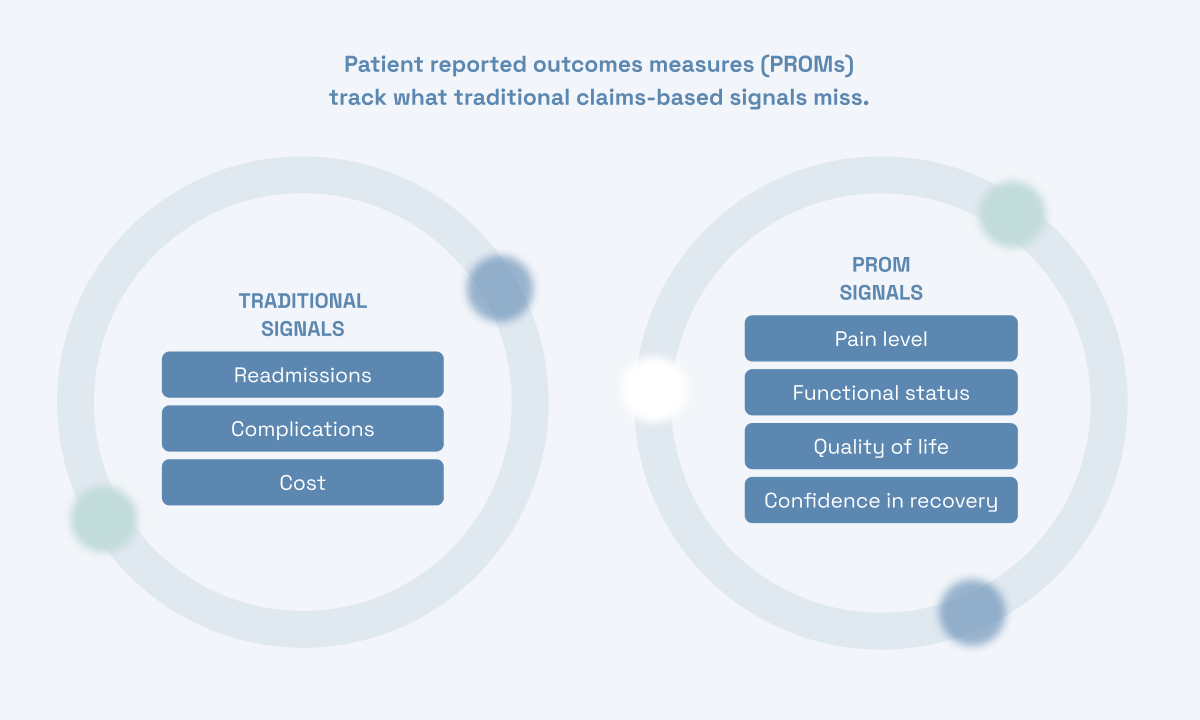
Why Claims Data Isn’t Enough
Traditional quality oversight in surgical care relies heavily on claims data—billing records that show readmissions, complications, and costs. This data is useful, but it has serious limitations.
First, it’s retrospective. Claims data typically arrives months after surgery. By the time you see that a patient was readmitted or had a complication from a claim, the window to intervene has long closed.
Second, it’s incomplete. Claims tell you whether something went wrong enough to generate another bill. They don’t tell you whether the patient is still in significant pain, whether they can climb stairs, whether they went back to work, or whether they feel the surgery was worth it. A patient can avoid readmission and still have a poor outcome. A patient can have no coded complication and still be struggling.
PROMs fill that gap. By asking patients directly about pain, function, and daily life at structured intervals during recovery, PROMs create visibility into the experience of care that no billing record can provide. And because they’re collected in real time, they can serve as an early warning system—flagging patients whose recovery is going off track before a readmission or complication ever shows up in a claim.
What This Looks Like in Practice
Imagine an employee who has knee replacement surgery. In a traditional model, they’re discharged, they go home, and unless something goes seriously wrong—an ER visit, a readmission—no one is systematically tracking how they’re doing.
In a model that uses PROMs, that same patient is asked at regular intervals: How is your pain when rising from a chair? How severe is knee stiffness when waking in the morning? ? What is the degree of difficulty when simply walking on a flat surface? These aren’t casual check-ins. They’re validated instruments that produce scores clinicians can act on.
When a patient’s PROM scores diverge from the expected recovery trajectory—say, pain isn’t improving at the rate it should —that signal can trigger clinical follow-up: a call from a nurse navigator, coordination with the surgeon, or an earlier office visit. The goal is to catch problems while they’re still small and manageable, rather than waiting until they become complications that require another procedure or another hospitalization.
Why This Should Be on Every Benefits Leader’s Radar
For employers, the value proposition of PROMs is straightforward. Complications and readmissions are among the biggest cost drivers in surgical care. Catching problems early reduces downstream utilization. Smoother recovery means faster return to work and less extended disability. And tracking whether surgeries actually produce the functional improvements patients were hoping for creates a level of accountability that claims data alone cannot provide.
But here’s the part that often gets missed: PROMs don’t just help individual patients. Over time, aggregated PROM data reveals patterns—which surgeons’ patients consistently recover well, which procedures reliably deliver functional improvement, and where care pathways need refinement. That kind of intelligence turns quality measurement from a backward-looking report card into a forward-looking system for improvement.
Research supports this. Studies in oncology have found that systematic PROM collection have led to earlier detection of symptoms, reduced emergency department visits, and even improved survival. In orthopedic care, Dartmouth-Hitchcock’s Spine Center has been collecting PROMs since the late 1990s, using the data to compare whether medical or surgical treatment is best for specific conditions—and sharing results with patients to inform better shared decision-making.
The Bottom Line
Most employer-sponsored surgical care is still measured by what went wrong, not by what went right. Claims data tells you about readmissions and costs. It doesn’t tell you whether your employee can pick up their child, walk up the stairs at home, or even dress themselves independently.
PROMs close that gap. They’re the only quality signal that captures what patients actually experience in recovery—and they’re the only one that arrives in time to do something about it. If your surgical benefits partner isn’t tracking PROMs, the question is simple: how would they know if the care is working?



